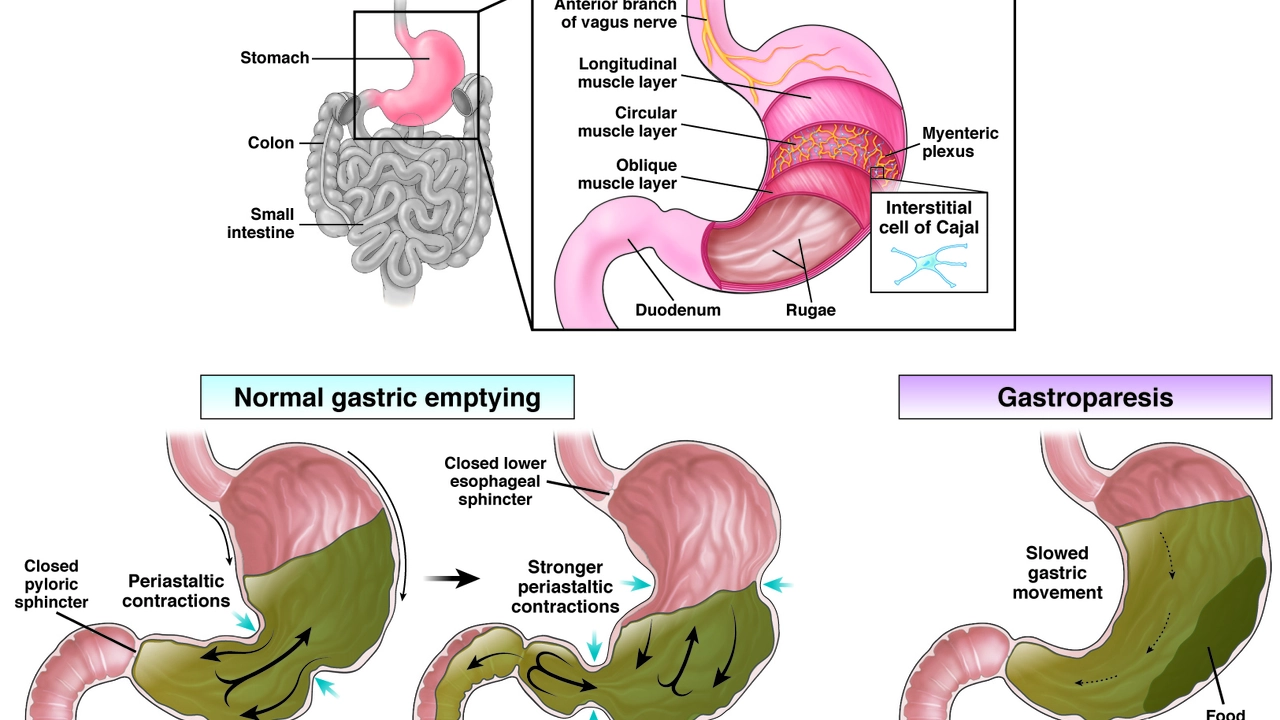
Diabetic Gastroparesis: What It Feels Like and What You Can Do
Diabetic gastroparesis happens when high blood sugar damages the nerves that move food through your stomach. That delay in stomach emptying leaves you bloated, full fast, nauseous, or vomiting — and it makes blood sugar harder to control. If you have diabetes and these symptoms, pay attention: this condition changes how you manage food and medication.
How to spot it
Common signs include early fullness after small meals, bloating, nausea, vomiting undigested food, heartburn, and unpredictable blood sugar swings. Weight loss and poor appetite also show up in more severe cases. If symptoms come on slowly after years of high blood sugar, nerve damage is often the reason.
Practical daily tips
Small, frequent meals are the easiest win. Try five to six small meals instead of three big ones. Choose low-fat, low-fiber foods because fat and fiber slow stomach emptying. Smooth, blended meals and liquid nutrition shakes often digest faster and give you steadier glucose control.
Cut down on high-fat snacks and raw vegetables that can sit in the stomach. Cooked, soft foods like soups, eggs, lean fish, and mashed potatoes usually work better. Chew thoroughly and avoid carbonated drinks that can increase bloating.
Check timing of diabetes meds with your provider. Gastroparesis makes blood sugar unpredictable, so insulin timing and dose may need adjustment. Continuous glucose monitoring (CGM) helps you see patterns and react faster to lows and highs.
Avoid medicines that slow stomach emptying when possible. Opioids, some anticholinergics, and certain diabetes drugs (GLP-1 agonists like semaglutide or exenatide) can make symptoms worse. Talk with your clinician before stopping or changing meds.
Stay hydrated and aim for gentle activity after meals, like a short walk. Light movement can help with digestion. Work with a dietitian or diabetes educator to make a plan that fits your tastes and glucose targets.
When to see your doctor and common tests
See a doctor if vomiting is frequent, you’re losing weight without trying, or your blood sugar is out of control. Tests usually start with a gastric emptying study (scintigraphy) to measure how fast your stomach empties. Other tests might include breath tests, endoscopy to rule out blockage, or imaging for other causes.
Treatment ranges from changing diet and glucose control to medications that speed up the stomach (prokinetics) or anti-nausea drugs. Some drugs can have side effects, so discuss risks with your provider. In severe cases, options include feeding tubes or gastric electrical stimulation.
Diabetic gastroparesis is manageable for many people once you spot the pattern and adjust food, meds, and habits. If your symptoms are new or worse, don’t wait — talk to your diabetes team so you can get a plan that keeps you eating, hydrated, and in better control of your blood sugar.