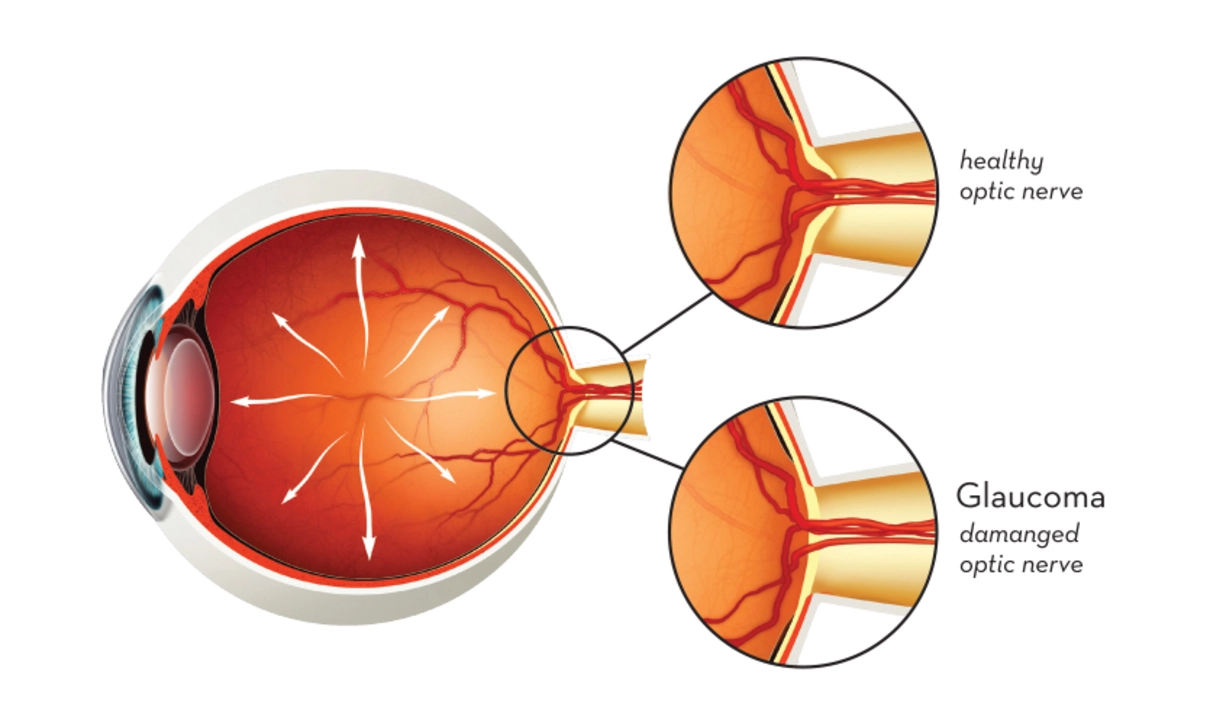
Glaucoma progression: how to slow vision loss
Glaucoma progression means your optic nerve is getting worse over time and vision is slowly shrinking. The most common driver is high eye pressure, but blood flow, genetics, and age also matter. The good news: most people can slow progression with treatment, regular checks, and simple daily habits.
First, know the signs to report right away. Early glaucoma often has no pain or visible symptoms. You might notice peripheral vision narrowing, trouble reading in dim light, or sudden contrast sensitivity change. If you already have glaucoma, sudden eye pain, nausea, or rapid vision loss are medical emergencies. Call your eye doctor if you see sudden changes.
Tests and tracking
Your eye doctor will use several tests to track progression. Tonometry measures eye pressure. Visual field tests map your side vision and show small changes over time. Optical coherence tomography, or OCT, takes a cross-sectional photo of the optic nerve and retina. Comparing these test results over months or years tells your doctor if your glaucoma is stable or progressing. Bring a list of all medications and any vision changes to each visit.
Treatments that slow progression
Lowering eye pressure is the main goal. Most people start with medicated eye drops that reduce fluid production or increase outflow. Common classes include prostaglandin analogs, beta blockers, alpha agonists, and carbonic anhydrase inhibitors. Take drops exactly as prescribed. Missing doses or using them unevenly increases the chance of progression.
If drops don’t reach target pressure, doctors may recommend laser treatments like selective laser trabeculoplasty (SLT). SLT can lower pressure for months or years and reduce the need for drops. For more advanced disease, minimally invasive glaucoma surgeries (MIGS) and traditional filtering surgeries create new outflow paths to lower pressure long term. Discuss risks and recovery times with your surgeon.
Beyond procedures, some practical steps help protect vision. Control blood pressure and blood sugar if you have hypertension or diabetes. Avoid smoking. Maintain a healthy weight and exercise moderately—walking and light cardio are good. Head-down positions for yoga and heavy weightlifting can raise eye pressure temporarily, so adapt exercises if advised by your eye doctor.
Supplements won’t replace treatment, but some people ask about omega-3s and antioxidants. Use supplements only after checking with your doctor to avoid drug interactions. Regular sleep, staying hydrated without over-drinking, and protecting eyes from direct sun and injury all help maintain eye health.
Keep a consistent eye exam schedule. For many patients with glaucoma or at risk, exams every 3 to 6 months matter. If tests show progression, your doctor will change the plan quickly to protect remaining vision. Early action gives the best chance to slow or stop progression. If you have questions about medications, side effects, or where to buy treatments safely, contact your pharmacy or eye care team for clear, practical advice.
Keep a written record of test numbers and dates. Share it with family and carry a copy to appointments to speed care decisions. Ask questions early always.