Pancreatic Duct Blockage & Malnutrition Risk Calculator
Enter your details and click "Calculate Risk Level" to see your risk assessment.
Interpretation Guide
This calculator estimates your risk level based on key clinical indicators. Higher scores indicate increased risk of malnutrition due to pancreatic duct blockage. Always consult with a healthcare provider for proper diagnosis and treatment.
When the pancreatic duct gets clogged, the body can’t absorb the nutrients it needs, and a silent cascade toward malnutrition begins. If you’ve ever wondered why some people with chronic abdominal issues keep losing weight despite eating enough, the answer often circles back to the pancreas - a tiny organ that does a huge job in digestion.
Quick Take
- Pancreatic duct blockage stops enzymes from reaching the gut, leading to exocrine pancreatic insufficiency (EPI).
- EPI causes fat malabsorption, steatorrhea, and progressive weight loss.
- Blood tests, imaging, and secretin‑stimulated MRCP are the main diagnostic tools.
- Treatment combines duct‑clearing procedures (ERCP), pancreatic enzyme replacement therapy (PERT), and targeted nutrition plans.
- Regular monitoring of weight, stool fat, and vitamin levels is essential to prevent long‑term malnutrition.
What Is Pancreatic Duct Blockage?
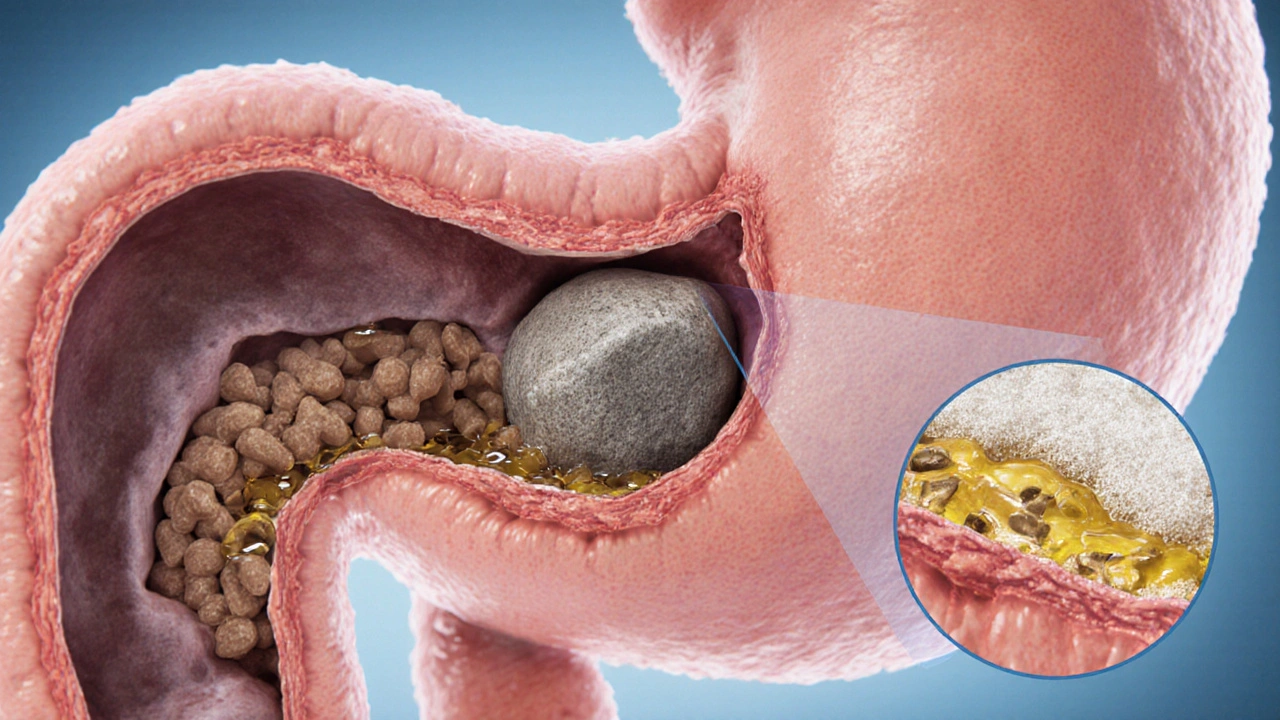
Pancreatic duct blockage is a condition where the main duct that carries digestive enzymes from the pancreas into the duodenum becomes obstructed by scar tissue, stones, or tumors. The blockage prevents enzymes from reaching the small intestine, crippling the organ’s exocrine function.
Why the Blockage Undermines Digestion
The pancreas produces a cocktail of enzymes - lipase, amylase, and proteases - that break down fats, carbs, and proteins. When the duct is clogged, these enzymes stay trapped inside the gland, a state known as exocrine pancreatic insufficiency (EPI).
EPI means the gut receives only a fraction of the enzymes it needs. Fat‑soluble vitamins (A, D, E, K) and essential fatty acids are especially vulnerable because they rely on lipase to be absorbed. The result is a classic pattern of steatorrhea (fatty, foul‑smelling stools) and gradual nutrient depletion.
How Malnutrition Develops
Malnutrition isn’t just “not eating enough.” It’s a mismatch between what you ingest and what your body actually absorbs. In the context of a clogged duct, three mechanisms drive the problem:
- Steatorrhea - undigested fat leaves the body, taking calories and vitamins with it.
- Protein breakdown is incomplete, leading to muscle wasting and lower serum albumin.
- Chronic inflammation from the blocked gland can raise metabolic rate, burning more calories than usual.
Patients often report unintentional weight loss of 5-10% of body weight within months, persistent fatigue, and bone pain from vitamin D deficiency.
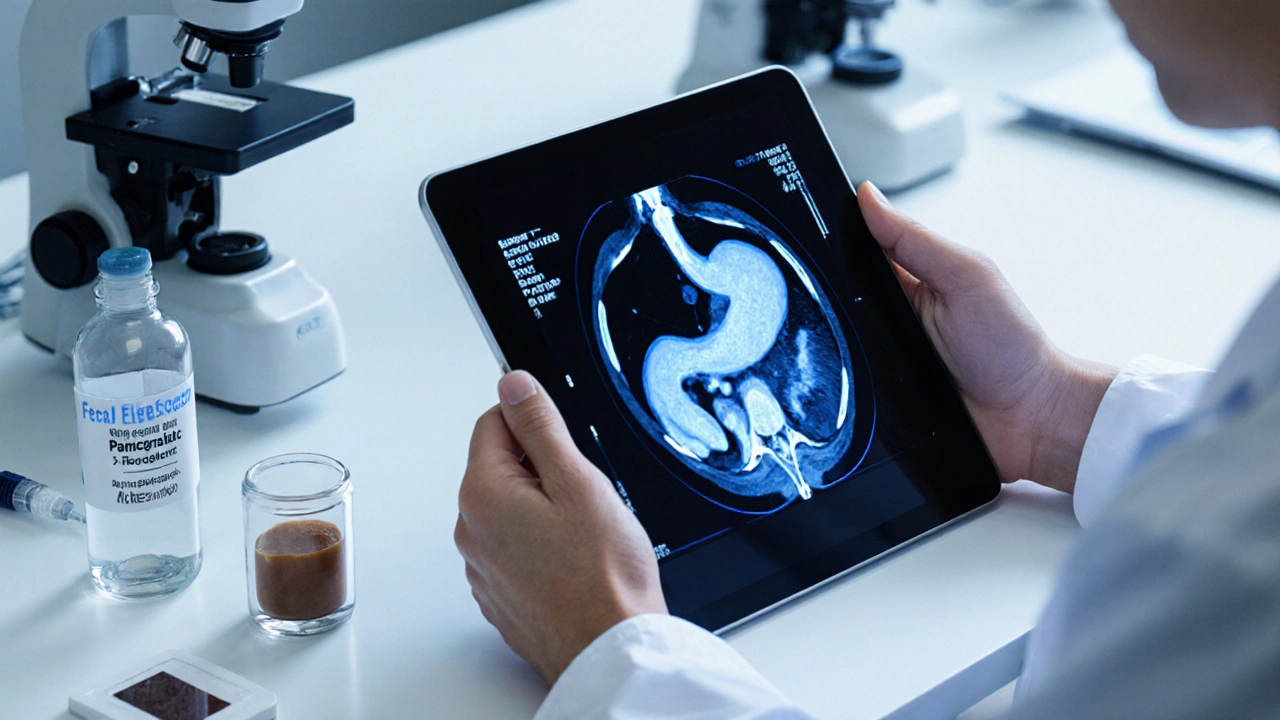
Diagnosing the Blockage‑Malnutrition Link
Because symptoms overlap with many gastrointestinal disorders, a systematic work‑up is crucial.
- Blood panels: Low fecal elastase‑1 (<200µg/g) is a reliable marker for EPI. Low serum levels of vitamins A, D, E, and K hint at malabsorption.
- Imaging: Abdominal MRI with secretin stimulation visualizes ductal dilation and obstruction. CT scans can reveal calcifications or tumors.
- Endoscopic retrograde cholangiopancreatography (ERCP): Endoscopic retrograde cholangiopancreatography not only confirms the blockage but can also provide therapeutic stenting.
- Stool analysis: Quantifying fat content (>7g per 24h) confirms steatorrhea.
Combining these tests paints a clear picture of how the duct obstruction is starving the body.
Treatment Options: Unblocking and Replacing Enzymes
Addressing the root cause and supporting digestion go hand‑in‑hand.
Procedural Interventions
When stones or strictures are the culprits, an ERCP can place a plastic or metal stent to restore flow. In chronic cases, surgical pancreaticojejunostomy (Puestow procedure) reroutes the duct to a nutrient‑rich part of the intestine.
Pancreatic Enzyme Replacement Therapy (PERT)
For many patients, especially those unable or unwilling to undergo invasive procedures, pancreatic enzyme replacement therapy is the cornerstone. The key is to match the lipase dose to the fat content of the meal - typically 500-1000lipase units per gram of fat.
Common PERT formulations (e.g., Creon, Zenpep) are enteric‑coated to survive stomach acid and release enzymes in the duodenum. Proper timing (with the first bite) maximizes absorption.
Nutrition Management
Even with enzymes, dietary tweaks speed recovery:
- Spread fat intake evenly across 5-6 small meals to avoid overwhelming the limited enzyme supply.
- Choose medium‑chain triglycerides (MCT oil) - they bypass the need for pancreatic lipase.
- Supplement fat‑soluble vitamins (A, D, E, K) and zinc, as deficiencies are common.
- Maintain high‑quality protein sources (lean meat, eggs, whey) to counter muscle loss.
Registered dietitians often recommend a baseline of 30-35kcal/kg body weight per day, adjusting upward as weight stabilizes.
Monitoring Progress and Preventing Relapse
Long‑term success hinges on regular follow‑up:
- Weigh-ins every 2-4 weeks until weight stabilizes.
- Fecal elastase or stool fat testing every 3 months to gauge enzyme efficacy.
- Serum vitamin panels every 6 months; adjust supplementation as needed.
- Imaging every 12-18 months for patients with chronic pancreatitis to catch new strictures early.
Patients who miss these checkpoints often slip back into malnutrition unnoticed.
Case Snapshot: From Blockage to Balanced Nutrition
John, a 58‑year‑old former smoker, presented with a 12‑kg weight loss, oily stools, and abdominal pain. Tests revealed a calcified stone blocking his main pancreatic duct. After an ERCP‑driven stent placement and initiation of PERT at 900lipase units per gram of fat, his stool fat dropped from 12g to 4g per day. Six months later, he regained 8kg, his vitamin D rose from 12ng/mL to 28ng/mL, and his energy levels improved dramatically. This turnaround underscores how quickly malnutrition can reverse once the duct is cleared and nutrition is re‑optimized.
| Cause | Typical Presentation | Primary Nutritional Consequence |
|---|---|---|
| Pancreatic duct stones | Intermittent abdominal pain, jaundice | Severe fat malabsorption → steatorrhea |
| Chronic pancreatitis fibrosis | Progressive pain, calcifications on CT | Gradual loss of enzymes → protein‑calorie malnutrition |
| Pancreatic head tumor | Weight loss, painless jaundice | Combined EPI and obstructive jaundice → multi‑micronutrient deficits |
| Strictures from prior ERCP | Recurrent pain after procedures | Variable fat malabsorption depending on stricture length |
Bottom Line
When the pancreatic duct is blocked, the body’s ability to digest and absorb nutrients collapses, often spiraling into serious malnutrition. Early detection through enzyme testing and imaging, followed by a combination of duct‑clearing procedures, enzyme replacement, and smart nutrition, can halt-and even reverse-this decline. Regular monitoring keeps the balance in check, ensuring patients stay nourished and healthy.

Frequently Asked Questions
What symptoms hint that a pancreatic duct blockage is causing malnutrition?
Typical clues include unexplained weight loss, oily or frothy stools (steatorrhea), frequent abdominal pain after meals, and fatigue despite eating normally. Low blood levels of fat‑soluble vitamins (A, D, E, K) also raise suspicion.
How reliable is fecal elastase as a test for exocrine pancreatic insufficiency?
Fecal elastase‑1 is non‑invasive and highly specific. Levels below 200µg/g indicate moderate to severe EPI, while values under 100µg/g reflect severe insufficiency. It’s most accurate when the patient isn’t on enzyme therapy.
Can diet alone fix the malnutrition caused by a blocked duct?
Diet helps, but without restoring enzyme flow the body can’t fully absorb nutrients. A low‑fat, MCT‑rich diet paired with PERT offers the best chance of reversing deficiencies.
Is ERCP safe for everyone with a duct blockage?
ERCP is effective but carries risks such as pancreatitis, infection, or perforation. It’s generally reserved for patients with symptomatic stones, strictures, or tumor‑related obstructions after evaluating the risk‑benefit profile.
How often should I get my vitamin levels checked after starting PERT?
Check vitamin A, D, E, and K at baseline, then repeat every 6 months. Adjust supplementation based on the results; most patients need higher doses of vitamin D and E during the first year.

Rachelle Dodge
October 2, 2025 AT 22:14Understanding how a blocked pancreatic duct starves the body of essential nutrients is vital. The cascade from enzyme loss to steatorrhea creates a silent hunger that many overlook. Early recognition of oily stools and unexpected weight loss can halt the march toward malnutrition. A simple blood test for fecal elastase often shines a light on the hidden problem.
Gaurav Joshi
October 11, 2025 AT 10:52From a clinical standpoint, the interplay of age, weight loss, and stool characteristics forms a reliable risk matrix. Chronic pancreatitis and ductal stones add substantial weight to the score, underscoring the need for imaging. Vitamin D deficiency frequently accompanies exocrine insufficiency, demanding routine supplementation. Coordinated care between gastroenterology and nutrition services yields the best outcomes.
Elaine Proffitt
October 19, 2025 AT 23:29Blockage stops enzymes reaching the gut causing fat to pass undigested it leads to oily stools and calorie loss without much pain
Christopher Munt
October 28, 2025 AT 11:07Wow this really hits home 😮! If your pancreas can’t drop the right enzymes your body feels the emptiness even after a big meal 🍽️. Enzyme pills and MCT oil can fill the gap 😊.
Mike Creighton
November 5, 2025 AT 23:45When the pancreatic duct clogs, the body embarks on a tragic odyssey of nutrient deprivation. The enzymes that should cascade into the duodenum are trapped, leaving fats untouched and calories unabsorbed. This invisible siege manifests as steatorrhea, a greasy, foul‑smelling stool that signals fat loss. Simultaneously, proteins are only partially broken down, accelerating muscle wasting. The chronic inflammation that often accompanies ductal obstruction further raises metabolic demand, burning calories like a furnace. Patients may lose five to ten percent of their body weight within months, despite eating what seems like ample portions. Vitamin A, D, E, and K tumble low because they hitch a ride on the very fats that now slip through the gut. The resulting deficiencies can cause night blindness, brittle bones, and impaired clotting, compounding the clinical picture. Diagnostic work‑up must therefore combine fecal elastase assays, serum vitamin panels, and cross‑sectional imaging such as MRCP. Once the blockage is identified, interventional endoscopy can restore flow by clearing stones or placing stents. In cases where surgery is warranted, a pancreaticojejunostomy re‑routes secretions to a healthier segment of intestine. Yet many patients cannot undergo invasive procedures, making pancreatic enzyme replacement therapy the cornerstone of management. The key to effective PERT is matching lipase units to the gram of fat in each meal, typically 500‑1000 units per gram. Coupled with a diet that spreads fat intake across multiple small meals and includes MCT oil, nutrient absorption improves dramatically. Ongoing monitoring of weight, stool fat, and vitamin levels ensures that the therapeutic window remains open, preventing the slow creep back into malnutrition.
Desiree Young
November 14, 2025 AT 12:23The duct blockage is a huge problem
Vivek Koul
November 23, 2025 AT 01:01In the context of exocrine pancreatic insufficiency, a systematic approach is indispensable. Initial laboratory assessment should include fecal elastase‑1 quantification, serum concentrations of fat‑soluble vitamins, and a comprehensive metabolic panel. Imaging modalities, notably secretin‑stimulated magnetic resonance cholangiopancreatography, delineate anatomical obstruction with high fidelity. Therapeutic intervention must be tiered: endoscopic stenting for calculi‑related strictures, surgical diversion for refractory fibrosis, and adjunctive pancreatic enzyme replacement therapy to compensate for residual insufficiency. Nutritional rehabilitation should be guided by a registered dietitian, emphasizing medium‑chain triglycerides, protein adequacy, and vitamin supplementation calibrated to serial laboratory results. Regular interdisciplinary review, at intervals of three to six months, mitigates the risk of relapse and preserves anthropometric stability.
Frank Reed
December 1, 2025 AT 13:39Hey there! just wanted to say that getting those enzyme pills on time can really turn things around. i’ve seen folks bounce back when they pair the meds with MCT oil and a few extra protein shakes. keep an eye on your weight and let the doc tweak the dose if needed. you’ve got this!
Bailee Swenson
December 10, 2025 AT 02:17Seriously, skipping the stent is nonsense 😡. If the duct stays blocked, you’re just inviting endless malnutrition. Get the ERCP done, pop the enzymes, and stop wasting time!
tony ferreres
December 18, 2025 AT 14:55Life’s most subtle betrayals often come from within, like a silent duct that refuses to cooperate 🌌. Ignoring that betrayal is tantamount to self‑sabotage, and the body will rebel with every ounce of lost weight 😤. Take action, or let the hidden enemy win.
Kaustubh Panat
December 27, 2025 AT 03:32While your dramatization captures the cascade vividly, it neglects the nuance of patient heterogeneity. Not every obstruction warrants an aggressive surgical route; a measured endoscopic approach often suffices. Moreover, the pharmacokinetics of lipase formulations demand individualized dosing rather than a blanket 500‑1000 U/g recommendation. A more discerning discourse would elevate the conversation beyond theatrical flair.
Arjun Premnath
January 4, 2026 AT 16:10Great summary! It’s essential to remember that regular follow‑up labs can catch vitamin deficiencies before clinical symptoms appear. Coordinating care between gastroenterology and nutrition ensures a holistic plan.
Johnny X-Ray
January 13, 2026 AT 04:48Whoa, the heat is on! 🔥 Your passion underscores a real danger, but let’s channel that fire into actionable steps: schedule that ERCP, start PERT, and monitor progress. Together we can tame the beast.
tabatha rohn
January 21, 2026 AT 17:26Enough drama, just get the enzymes! 😤
Mark Rohde
January 30, 2026 AT 06:04The philosophical musings are noted, but the gut doesn’t care about existential angst. It craves enzymes, and without them, the body collapses. Spare the poetry and prescribe the therapy.
Rajan Desai
February 7, 2026 AT 18:42Observing the pattern, patients with chronic pancreatitis often exhibit a progressive decline in elastase values, correlating with increasing steatorrhea severity.
S O'Donnell
February 16, 2026 AT 07:20In assessing the pathophysiology of pancreatic duct obstruction, one must first appreciate the anatomical continuity between the pancreatic secretory apparatus and the duodenal lumen. The cessation of enzyme flow precipitates a cascade wherein dietary lipids remain emulsified yet unhydrolyzed, ultimately forming globules that escape absorption. Consequently, each gram of unabsorbed fat represents a caloric deficit approximating nine kilocalories, inexorably contributing to weight loss. Concurrently, the maldigestion of fat‑soluble vitamins precipitates a secondary deficiency syndrome, characterized by osteomalacia, coagulopathy, and visual disturbances. The clinical manifestation of steatorrhea, often described as pale, malodorous, and frothy stools, provides a tangible clue to this underlying insufficiency. Laboratory quantification of fecal elastase‑1 offers a non‑invasive metric, with values below 200 µg/g denoting moderate to severe exocrine insufficiency. Imaging, particularly secretin‑enhanced MRCP, delineates ductal strictures, calculi, or neoplastic encroachments with high resolution, guiding therapeutic decisions. Endoscopic retrograde cholangiopancreatography remains the cornerstone for mechanical relief, allowing stent placement or stone extraction. When endoscopic modalities fail or are contraindicated, surgical options such as lateral pancreaticojejunostomy warrant consideration, albeit with an elevated risk profile. Pharmacologic supplementation with enteric‑coated pancreatic enzyme preparations restores digestive capacity, provided dosing is calibrated to the gram of dietary fat ingested. Nutritional rehabilitation should emphasize medium‑chain triglycerides, which bypass pancreatic lipase dependency, alongside high‑quality protein sources to mitigate sarcopenia. Periodic reassessment of weight, serum vitamin levels, and stool fat content ensures that therapeutic efficacy is sustained and adjustments are made in a timely fashion.
Yamunanagar Hulchul
February 24, 2026 AT 19:58Wow!!! This is an eye‑opener!!! 🌟 The pancreas, that tiny powerhouse, can cause a massive ripple when its duct gets clogged!!! Fat malabsorption, vitamin loss, weight drop – all happen like dominoes!!! The good news? With the right combo of ERCP, enzyme pills, and a diet rich in MCT oil, you can flip the script!!! Keep tracking your weight, get those labs checked, and celebrate every gram of fat you finally absorb!!! 🎉
Sangeeta Birdi
March 5, 2026 AT 08:36Sending positive vibes! 🌈 Remember, consistent enzyme use and regular check‑ups can make a huge difference. Celebrate small wins, like a steadier weight or brighter skin, and keep the momentum going! 😊
Chelsea Caterer
March 13, 2026 AT 21:14Take action early and you can avoid big set backs